Visceral Fat: Healthy Levels and How a DEXA Scan Measures It Accurately
Visceral fat, the deep abdominal fat that wraps around your liver, pancreas and intestines, is one of the most clinically important numbers on a body composition report. Unlike the fat you can pinch beneath the skin, visceral adipose tissue (VAT) sits behind the abdominal wall and is metabolically active, releasing inflammatory signals that raise your risk of cardiovascular disease, type 2 diabetes and non-alcoholic fatty liver disease.
This guide, written by Dr Emil Gadimali, explains what counts as a healthy visceral fat level, how a DEXA scan measures VAT to clinical-grade accuracy, and the evidence-based options available if your reading is higher than it should be.
Quick answer
- A healthy visceral fat mass on DEXA is typically under around 1 kg for women and under around 1.5 kg for men, though laboratory reference ranges vary by device and population.
- Visceral fat behaves very differently from subcutaneous fat and carries a higher cardiometabolic risk at the same overall body fat percentage.
- A DEXA body composition scan reports VAT in grams using a validated algorithm, far more precisely than BMI or a tape-measure waist reading.
- Reducing visceral fat is possible with sustained weight loss, resistance training, improved diet quality and, where clinically indicated, doctor-led medication.
What Is Visceral Fat?
Visceral fat is the adipose tissue packed inside the abdominal cavity, wrapped around internal organs such as the liver, pancreas, stomach and intestines. Clinicians sometimes call it intra-abdominal fat or, when reported on imaging, visceral adipose tissue (VAT). It sits behind the abdominal muscles, which is why a person with a protruding, firm belly can have a great deal of visceral fat even when subcutaneous fat stores appear modest.
Functionally, visceral fat is not simply a passive energy store. It is an active endocrine organ that secretes hormones and inflammatory chemicals, known as adipokines and cytokines, directly into the portal circulation supplying the liver. Elevated visceral fat therefore has a disproportionate effect on hepatic insulin sensitivity and systemic inflammation compared with peripheral fat stores.
According to the NHS, a large waist circumference is one of the clearest clinical signs of excess visceral fat, even when body weight appears within the normal BMI range.
Why High Visceral Fat Matters for Your Health
Excess visceral fat is strongly associated with the metabolic conditions that drive premature mortality in the United Kingdom. A 2019 consensus statement in Nature Reviews Endocrinology concluded that visceral adiposity, rather than overall body weight, is the dominant driver of cardiometabolic risk in people living with obesity.
- Cardiovascular disease: VAT is linked to higher blood pressure, adverse lipid profiles and an elevated risk of heart attack and stroke, independent of BMI.
- Type 2 diabetes and insulin resistance: Inflammatory mediators released by visceral fat impair the body’s ability to respond to insulin, a primary mechanism underlying type 2 diabetes.
- Non-alcoholic fatty liver disease (NAFLD/MASLD): Because visceral fat drains via the portal vein, the liver is exposed to high concentrations of free fatty acids, which can trigger steatosis, inflammation and, eventually, fibrosis.
- Certain cancers: Cancer Research UK lists excess body fat as a recognised risk factor for 13 types of cancer, with central adiposity (a proxy for visceral fat) carrying particular weight in colorectal, endometrial and post-menopausal breast cancer.
The important clinical point is that someone can look slim, have a normal BMI and still carry dangerous levels of visceral fat. This phenotype, sometimes called TOFI (thin outside, fat inside), only becomes visible with a body composition measurement such as a DEXA scan.
What Counts as a Healthy Visceral Fat Level?
A DEXA scan reports visceral fat in grams (or kilograms), measured across a standardised region of the abdomen. The exact reference ranges differ between devices and populations, but the following thresholds, derived from peer-reviewed work using Hologic DEXA systems, are useful guides for UK adults.
- Women: below around 1,000 g is considered low risk. 1,000 to 1,600 g is an intermediate range where lifestyle change is advisable. Above 1,600 g is typically regarded as clinically elevated.
- Men: below around 1,500 g is considered low risk. 1,500 to 2,500 g is intermediate. Above 2,500 g is generally classed as clinically elevated, and above 3,000 g is high risk.
These numbers should be interpreted alongside waist circumference, fasting glucose, lipids and family history. The International Diabetes Federation uses a waist threshold of 80 cm in women and 94 cm in men of European descent as one criterion for metabolic syndrome, which broadly aligns with the DEXA figures above.
If you already have a DEXA report and want to understand how your results fit against these ranges, it can help to review the numbers with a clinician rather than compare against an online calculator alone.
How a DEXA Scan Measures Visceral Fat
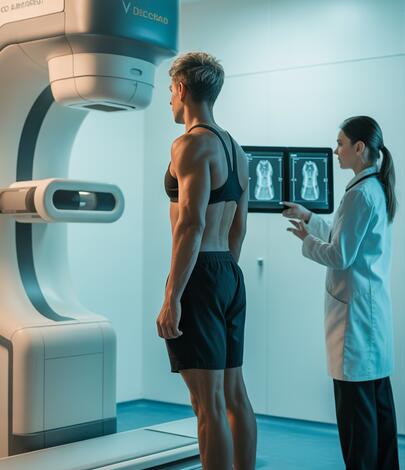
Dual-energy X-ray absorptiometry (DEXA) was originally developed to measure bone mineral density. Modern DEXA systems now use paired low-dose X-ray beams to differentiate bone, lean tissue and fat tissue across the whole body, at high spatial resolution and with a radiation dose similar to a trans-Atlantic flight.
To estimate visceral fat, the scanner software isolates a narrow abdominal region of interest (typically around the L4 to L5 lumbar level) and uses a validated algorithm to separate subcutaneous fat (outside the abdominal wall) from deeper, intra-abdominal fat. Published validation studies have shown correlation coefficients of R² > 0.93 between DEXA-derived VAT and the gold-standard CT measurement, at a fraction of the radiation dose.
Because the measurement is quantitative and reproducible, visceral fat on DEXA is one of the most useful numbers for tracking progress during a weight loss or metabolic health programme. You can read more about how DEXA scanning works and what a typical appointment involves.
Visceral Fat vs Subcutaneous Fat: Why the Distinction Matters
Subcutaneous fat is the familiar layer of fat that sits directly beneath the skin and can be pinched on the thighs, hips, arms and abdomen. Although it stores excess energy, subcutaneous fat is relatively metabolically quiet and, in moderation, appears to be at worst neutral for long-term health. Gluteofemoral fat, the type stored on the hips and thighs, may even be mildly protective against cardiometabolic disease.
Visceral fat, in contrast, is highly metabolically active. It drains directly into the liver, releases free fatty acids and inflammatory cytokines, and interferes with normal insulin signalling. That is why two people with identical body weight and identical BMI can have very different risk profiles: the distribution of fat, not just the amount, determines the clinical picture.
Simple measurements such as waist circumference are useful proxies but are blunt. A DEXA scan quantifies both depots separately and reports them alongside total body fat percentage, lean mass and bone density, giving a much richer picture.
What to Do if Your DEXA Scan Shows Elevated Visceral Fat
An elevated visceral fat reading is not an emergency, but it is an actionable finding. The evidence consistently shows that visceral fat is the fat depot most responsive to lifestyle intervention: weight loss through a sustained caloric deficit preferentially reduces VAT before subcutaneous fat, particularly during the first six to twelve weeks of a programme.
For some patients, however, lifestyle change alone is not enough, either because of genetic predisposition, hormonal factors such as the menopause, or because previous attempts have not been successful. In those cases, GLP-1 and GIP agonist medications (including Mounjaro, Wegovy and Ozempic) can produce substantial, clinically meaningful reductions in visceral fat when prescribed and monitored by a qualified doctor.
Weight management next step
If your DEXA results point to elevated visceral fat or metabolic risk, a supervised weight-loss programme may be worth considering. CutKilo, the sister service to DEXA London, offers doctor-led Mounjaro treatment from Dr Emil Gadimali, with dietitian support and regular clinical review throughout. DEXA scans are an ideal way to track body composition changes across a course of treatment, verifying that weight loss is predominantly fat, and specifically visceral fat, rather than lean muscle.
Evidence-Based Ways to Reduce Visceral Fat
The strategies with the strongest evidence base for reducing visceral fat are, predictably, the ones most often ignored because they are not glamorous. The list below is drawn from NICE guidance on obesity management, the NHS Better Health programme and a body of peer-reviewed trials.
- Sustained caloric deficit: even a modest 5 to 10% weight loss typically produces a disproportionate reduction in visceral fat, often 20 to 30%.
- Resistance training two to three times a week: preserves lean muscle, maintains resting metabolic rate and independently reduces VAT, even without significant weight change.
- Moderate to vigorous aerobic exercise: roughly 150 to 300 minutes per week, in line with NHS physical activity guidelines.
- Dietary quality: a higher intake of fibre, protein and whole foods, and a lower intake of ultra-processed foods and added sugars. There is no single magic diet, but quality matters more than label trends.
- Sleep: consistently sleeping fewer than six hours is associated with increased abdominal adiposity, partly through effects on appetite-regulating hormones.
- Alcohol reduction: alcohol is calorically dense and, through its effect on the liver, can directly worsen visceral fat storage.
- Medical options, when appropriate: GLP-1 and GIP agonist therapy, prescribed and monitored by a registered doctor, has been shown to reduce visceral fat substantially in adults who meet clinical criteria.
Tracking progress with a repeat DEXA scan every three to six months allows you, and your clinician, to verify that the changes are happening where they matter. Weight on a bathroom scale cannot tell you whether your visceral fat has fallen or whether you are losing muscle rather than fat.
Frequently Asked Questions
Is visceral fat the same as a beer belly?
Not exactly. A protruding abdomen can reflect a mixture of visceral fat, subcutaneous fat, abdominal bloating and weak core musculature. The only way to separate them reliably is with a DEXA scan or cross-sectional imaging.
Can thin people have high visceral fat?
Yes. This is the TOFI phenotype, short for thin outside, fat inside. Someone with a BMI of 22 can still carry clinically elevated visceral fat, which is why the scan matters even in people who appear to be a healthy weight.
How quickly can visceral fat change?
Visceral fat is the fat depot most responsive to intervention. Measurable reductions often occur within six to twelve weeks of a sustained caloric deficit, structured exercise or supervised medication, often before changes become visible in the mirror.
Does a DEXA scan show visceral fat in grams?
Yes. Modern DEXA systems report visceral adipose tissue in grams (or kilograms), along with a separate figure for subcutaneous fat in the abdominal region. The report also includes total body fat percentage, regional fat distribution and lean mass.
How often should I have a DEXA visceral fat scan?
For most adults making lifestyle changes, every three to six months is a reasonable cadence. For patients on GLP-1 treatment or in structured weight loss programmes, scans are often done at baseline, at three months and at twelve months to quantify progress.
Is a DEXA scan safe?
DEXA uses a very low dose of ionising radiation, typically less than a tenth of a standard chest X-ray and comparable to a single trans-Atlantic flight. It is considered safe for most adults. It is not used routinely in pregnancy.
Book a DEXA Visceral Fat Scan on Harley Street
DEXA London offers full-body composition and bone density scans at our Harley Street clinic in central London, reported by Dr Emil Gadimali. Results include quantitative visceral fat, total and regional body fat percentage, lean mass distribution, and bone density.
To book a DEXA scan, visit our booking page or call the clinic on 0207 637 8227. Appointments are typically available within a week and the scan itself takes around ten minutes.
Reviewed by Dr Emil Gadimali, MBBS, Clinical Director, DEXA London.